Revolutionizing Healthcare
The Promise and Potential of Clinical Decision Support Systems (CDSS)
30%
Increase in Patients Treated
30%
Improvement in Patient Satisfaction
30%
Reduction in Diagnostic Errors

Executive Summary
This case study investigates the transformative potential of implementing a Clinical Decision Support System (CDSS) in India’s public healthcare sector. Addressing critical issues such as the low doctor-patient ratio, diagnostic errors, and operational inefficiencies, CDSS offers a promising solution through AI-driven support. Drawing on previous successful implementations and outlining a detailed methodology for effective deployment, this study underscores how CDSS can enhance healthcare delivery, improve patient outcomes, and streamline operational costs.
Introduction
i. The Current State of Healthcare in India
India’s healthcare system faces significant challenges, with a doctor-patient ratio of 1:1668, far below the WHO-recommended 1:1000. The public healthcare sector is particularly strained, as only 10% of doctors serve in this domain. This leads to one government allopathic doctor for every 10,189 people. Additionally, the country has only one government hospital bed for every 2,046 people and one state-run hospital for every 90,343 people.
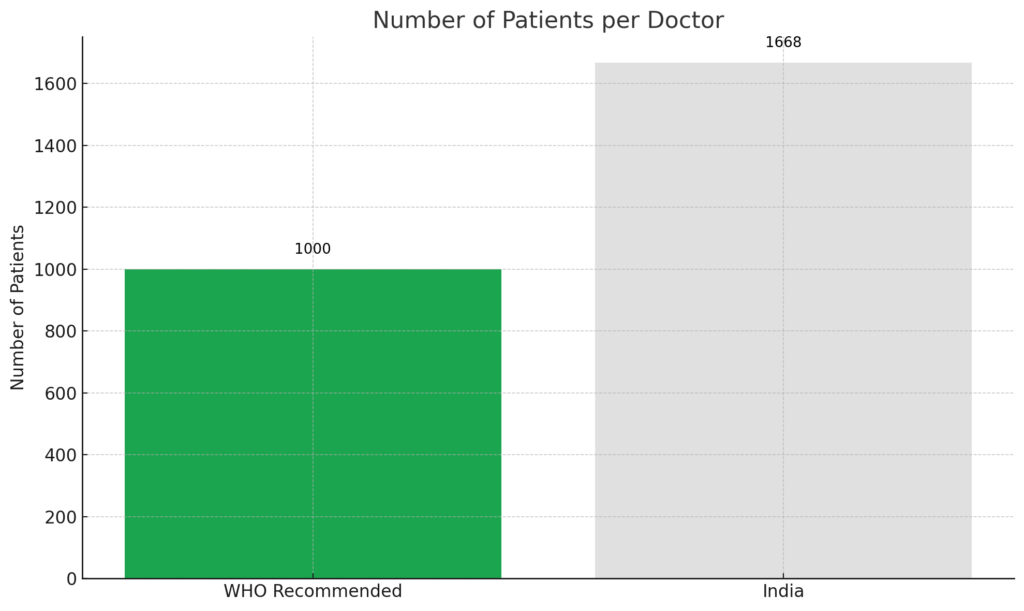
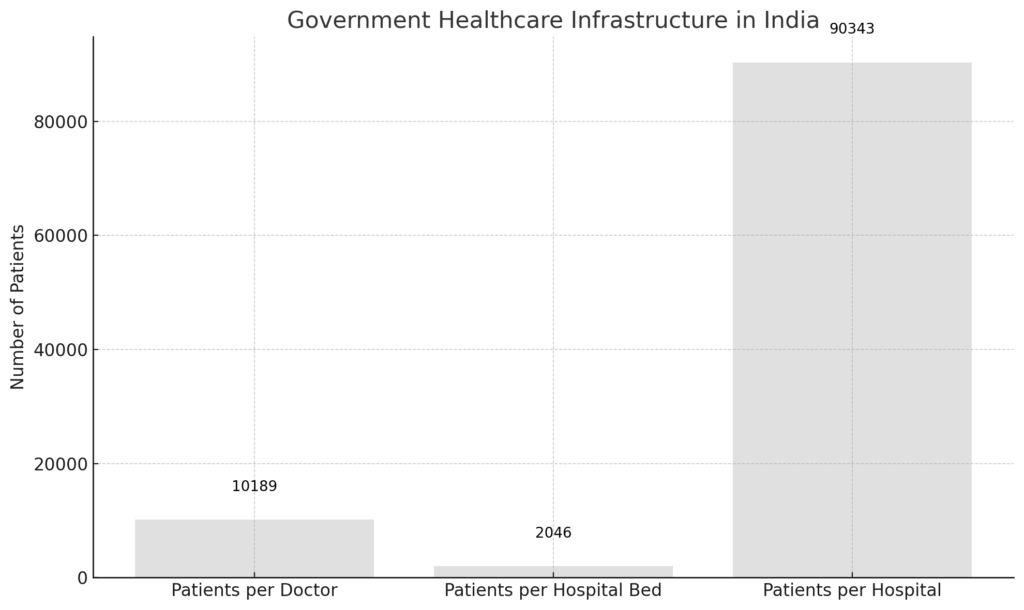
ii. Losses Due to Current Methodologies
The existing healthcare delivery model leads to inefficiencies, high costs, and poor patient outcomes. Diagnostic errors, redundant tests, and inadequate preventive care measures are prevalent, causing significant losses both financially and in terms of patient health .
iii. The Potential of AI and CDSS
Artificial Intelligence (AI), specifically through Clinical Decision Support Systems (CDSS), offers a viable solution to these challenges. CDSS can enhance diagnostic accuracy, streamline treatment processes, and provide real-time data analysis, leading to improved healthcare delivery and patient outcomes.
Successful CDSS Implementations: Learning from the Past
i. Telepsychiatry Project in Chandigarh
The Postgraduate Institute of Medical Education and Research (PGIMER) in Chandigarh implemented a knowledge-based CDSS for psychiatric disorders as part of their telepsychiatry project. This system provided diagnostic support and treatment recommendations, significantly improving diagnostic concordance among clinicians and ensuring consistent, high-quality care.
ii. mHealth Initiative in Andhra Pradesh
In Andhra Pradesh, a mobile CDSS was deployed to combat cardiovascular disease (CVD) in rural areas. The system enabled non-physician healthcare workers to provide effective care by offering diagnostic and treatment support. Despite system-level barriers, the initiative demonstrated the potential of CDSS to transform healthcare delivery in resource-limited settings.
Effective Implementation of CDSS in India
i. Implementation Strategy
Phase 1: Pre-Pilot Research (2 Weeks)
- Site Visits: Visit local government hospitals to understand current workflows.
- Expert Consultations: Engage with domain experts and hospital management to assess technology adoption challenges.
- Stakeholder Buy-in: Secure support from key stakeholders and identify counterparts for integration.
Phase 2: Pilot Implementation (20 Weeks)
- Dataset Training Feasibility Research (2 Weeks): Assess the feasibility of training AI models with available data.
- Pilot Deployment (18 Weeks): Implement CDSS in selected hospitals, focusing on outpatient departments.
ii. Key Components
- Manned Health Kiosks: Collect patient vitals and preliminary information, aiding in initial diagnostics.
- Central Data Repository: Securely store and manage patient data, ensuring easy access and integrity.
- Monitored Rule Engines: Oversee AI performance, ensuring continuous improvement and accuracy.
- Doctor Decision Support Systems: Provide comprehensive patient data and AI-driven diagnostic suggestions to doctors.
iii. Objectives and Targets
- Increase Patient Treatment by 30%: Streamline workflows and reduce the cognitive load on doctors.
- Improve Patient Satisfaction by 30%: Enhance diagnostic accuracy and provide personalized care.
- Reduce Diagnostic Errors by 30%: Utilize AI-driven insights to minimize human error.
- Decrease Untreated Patients by 30%: Improve healthcare access and outreach.
- Reduce Costs by 30%: Eliminate redundancies and optimize resource utilization.
Anticipated Outcomes and Impact
i. Improved Healthcare Delivery
The successful implementation of CDSS is expected to revolutionize healthcare delivery in India. By enhancing diagnostic accuracy and streamlining treatment processes, CDSS can significantly improve patient outcomes and satisfaction. The system will also reduce operational costs by minimizing redundant tests and optimizing resource use.
ii. Statistical Impact
- 30% Increase in Patients Treated: More efficient utilization of medical resources.
- 30% Improvement in Patient Satisfaction: Better diagnostics and personalized care plans.
- 30% Reduction in Diagnostic Errors: AI-driven insights to support accurate diagnoses.
- 30% Decrease in Untreated Patients: Enhanced accessibility and outreach.
- 30% Cost Reduction: Lower operational costs through optimized processes.
iii. Industry-Wide Impact
The pilot project will serve as a model for scaling CDSS across India, showcasing the transformative potential of AI in healthcare. Successful implementation will set a precedent for broader adoption, ultimately improving the overall healthcare landscape.
Conclusion
The integration of CDSS in India’s public healthcare system holds immense potential to address systemic inefficiencies and improve patient care. By leveraging AI, healthcare providers can enhance diagnostic accuracy, streamline treatment processes, and reduce operational costs. The successful implementation of CDSS will not only improve patient outcomes but also pave the way for future advancements in healthcare technology.
